- Usage
- Usage Cases
- Рressure ulcers
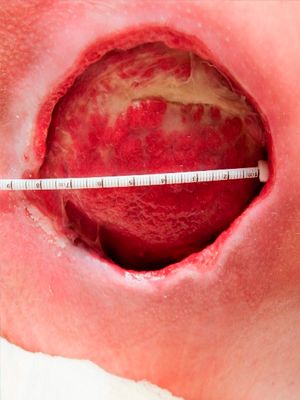
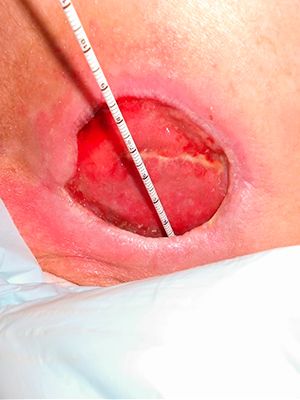
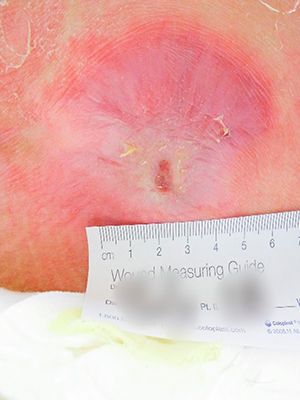
Case №32
Pressure Injury
Age of Wound: 4 months
USA
-
Gender:
Man
-
Age:
44 years
-
Diagnosis:
Pressure Injury
Рressure ulcers
The most important factors contributing to the formation of pressure ulcers are: continuous pressure, shearing forces, friction and moisture. Limited physical activity of patients, inadequate nutrition and care, urinary and fecal incontinence, comorbidities such as diabetes mellitus, Parkinson's disease, paraplegia, and wasting also play an important role in the development of ulcers.
Prolonged exposure to continuous pressure leads to local tissue ischemia. Muscle fibers are more sensitive to ischemic factors than skin. Changes in response to pressure develop primarily in the muscle layer above the bony prominence. Subsequently, they spread towards the skin. When the head of the bed is raised, when the patient's torso slides down, pressure is transferred to the sacrum and deep fascia. The forces of displacement in this case lead to tension and bending of the vessels, causing their thrombosis and damage to the skin. The combined action of displacement forces and continuous pressure can lead to the development of pressure ulcers even with low external pressure.
Classification of ultra ultra and risk assessment of their formation
Currently, there are many classifications of pressure ulcers.
5 stages:
-
1. Superficial bedsore
-
2. Deep bedsore
-
3. Deep bedsore with side pockets
-
4. Deep bedsore with osteomyelitis of the underlying bones
-
5. Scar bedsore
Distinguish between exogenous and endogenous bedsores
Bedsores can be superficial or deep.Deep pressure sores often go unnoticed until the top layers of the skin are affected. In the development of exogenous pressure ulcers, the main role is played by the factor of intense prolonged compression of soft tissues. Distinguish between external and internal exogenous bedsores.
External bedsores often occur in places where there are no muscles between the skin under pressure and the underlying bone (for example, in the back of the head, shoulder blades, femoral condyles, olecranon, sacrum, etc.). As a rule, such bedsores are observed in operated or traumatological patients who have been in a forced-immobilized position for a long time. The immediate causes of exogenous pressure ulcers are improperly applied plaster casts or splints, inaccurately fitted prostheses, corsets and medical orthopedic devices, as well as folds of clothing and sheets, tight bandages, etc.
Internal exogenous pressure ulcers are formed under rigid drains, catheters, which remain in a wound, cavity or organ for a long time. Endogenous pressure ulcers develop with severe neurotrophic disorders and circulatory disorders. Mixed and neurotrophic endogenous pressure ulcers are conventionally distinguished. Mixed bedsores are found in debilitated emaciated patients who are unable to independently change the position of the body or limbs. Endogenous neurotrophic pressure ulcers occur in patients with damage to the spinal cord or large nerves, stroke, or a brain tumor.In connection with a violation of innervation, severe neurotrophic disorders develop in tissues, including in the skin.
With external bedsores, there are three stages:
- The stage of circulatory disorders (stage I) is characterized by local blanching of the skin, which is replaced by cyanosis, the tissues become swollen and cold to the touch. Then bubbles appear, which, merging, lead to the detachment of the epidermis.
- In the stage of necrotic changes and suppuration (stage II), necrosis of the skin and underlying tissues (tissue, fascia, etc.) occurs. With exogenous pressure ulcers, dry necrosis is more often formed, and with endogenous pressure ulcers, wet gangrene usually develops with progressive necrosis of the surrounding tissues.
- In the healing stage (stage III), with a favorable development of the process, the wound is cleared of necrotic tissues, covered with granulations, followed by scarring or epithelization. Pressure ulcers often lead to complications. The most serious of these is sepsis.
Cooperate With Us
or via contact phones or email
-
Conveniently
By contacting only one supplier, our customers receive a wide range of products in the shortest possible time.
-
Simple
Our customers are only required to form an order for the supply of products, we will take care of all further tasks
-
Profitable
We save our customers money on import
and delivery taxes